FDA AI Diagnostic Device Draft Rules: Bias Assessment for Imports
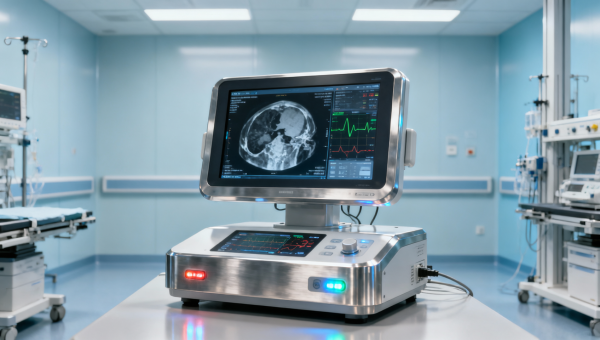
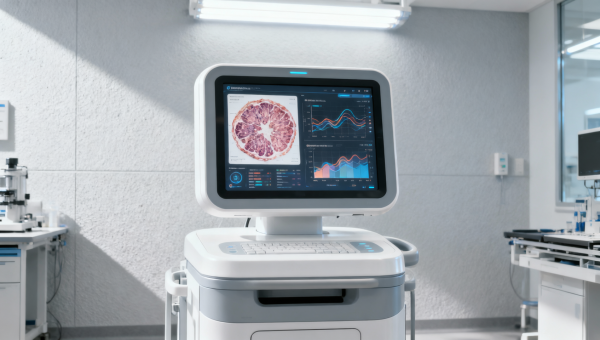
FDA released a draft regulatory guidance on April 20, 2026, requiring algorithmic bias impact assessments for imported AI-based diagnostic medical devices — including medical imaging analyzers and remote ECG interpretation terminals. This development directly affects international manufacturers, importers, and regulatory affairs teams serving the U.S. market, as it introduces a new premarket submission requirement with tangible operational and compliance implications.
Event Overview
On April 20, 2026, the U.S. Food and Drug Administration (FDA) published the Draft Guidance for Industry and FDA Staff: Artificial Intelligence/Machine Learning (AI/ML)-Based Software as a Medical Device (SaMD) Regulatory Framework. Effective beginning Q3 2026, all importers seeking 510(k) clearance or De Novo classification for AI/ML-based diagnostic devices must submit an Algorithmic Bias Impact Report (AI Bias Impact Report) concurrently with their application. The report must include clinical performance analysis across at least three demographic subgroups — race, sex, and age — using real-world or representative clinical data.
Which Subsectors Are Affected
Direct Trade Enterprises (Importers & U.S. Agent Firms)
These entities are directly responsible for regulatory submissions to FDA and will bear primary accountability for the completeness and validity of the AI Bias Impact Report. Their role shifts from document coordination to active oversight of bias evaluation methodology, data sourcing, and subgroup stratification — increasing both technical due diligence and timeline risk.
Medical Device Manufacturers (Non-U.S. Based)
Overseas manufacturers supplying AI-assisted diagnostic equipment to the U.S. market must now generate, validate, and document bias-related performance data prior to submission. This adds upstream R&D and clinical validation requirements — particularly where historical training datasets lack sufficient demographic diversity or real-world deployment records across subgroups.
Regulatory Affairs & Clinical Validation Service Providers
Firms offering regulatory strategy, clinical study design, or analytical validation support will see increased demand for expertise in fairness-aware ML evaluation — including statistical methods for subgroup performance comparison (e.g., sensitivity/specificity differentials), dataset representativeness assessment, and audit-ready reporting frameworks.
What Relevant Enterprises or Practitioners Should Focus On — And How to Respond Now
Monitor official updates to the draft guidance and related FDA communications
The current version is a draft. Final requirements may adjust scope (e.g., device classification thresholds), acceptable methodologies, or reporting format. Stakeholders should track FDA’s public docket (Docket No. FDA-2026-N-XXXXX) and upcoming stakeholder webinars scheduled for Q2 2026.
Identify high-priority product categories and submission timelines
Devices falling under 510(k) or De Novo pathways — especially those performing image-based diagnosis (e.g., diabetic retinopathy detection, lung nodule analysis) or waveform interpretation (e.g., arrhythmia classification) — are explicitly in scope. Companies planning submissions between July–December 2026 should treat bias assessment as a critical path item, not an add-on.
Distinguish policy signal from implementation readiness
Analysis来看, this requirement signals FDA’s institutional shift toward proactive bias governance — but does not yet specify approved tools, reference benchmarks, or minimum sample sizes per subgroup. Current best practice is to align with NIST AI Risk Management Framework (AI RMF) v1.1 and ISO/IEC 23053 for ML system documentation, rather than await formal FDA endorsement.
Initiate internal cross-functional alignment and data inventory
Manufacturers and importers should convene regulatory, clinical, data science, and quality teams now to map existing clinical datasets against required subgroups, assess gaps in demographic annotation, and determine whether supplemental collection or third-party augmentation is needed — especially for age-stratified performance in pediatric or geriatric populations.
Editorial Perspective / Industry Observation
From industry perspective, this draft is best understood as a formalized policy signal — not an immediate enforcement mandate. While the Q3 2026 effective date is fixed, FDA has historically allowed phased adoption for novel requirements, particularly where standardized evaluation methods remain under development. Observation来看, the emphasis on *clinical performance differentials* (not just training data composition) suggests FDA intends to assess real-world equity outcomes — a notable evolution beyond transparency or documentation alone. Current more appropriate framing is that this represents the beginning of enforceable bias accountability in SaMD regulation, not its fully matured form.
Conclusion
This draft guidance marks a structural inflection point in U.S. AI medical device regulation: bias assessment transitions from voluntary best practice to mandatory premarket submission content. For stakeholders, it is neither a sudden disruption nor a distant concern — rather, it is a defined, time-bound requirement demanding targeted preparation. The most constructive stance is to treat it as an operational milestone within existing regulatory workflows, not a standalone compliance event.
Information Sources
Main source: U.S. FDA, Draft Guidance Document “Artificial Intelligence/Machine Learning (AI/ML)-Based Software as a Medical Device (SaMD) Regulatory Framework”, issued April 20, 2026. Docket ID pending publication; publicly available via FDA’s Guidance Documents portal. Note: Final guidance text, effective dates for specific device types, and acceptance criteria for bias reports remain subject to revision and ongoing stakeholder feedback through the comment period ending August 15, 2026.
Recommended News
Popular Tags
Global Trade Insights & Industry
Our mission is to empower global exporters and importers with data-driven insights that foster strategic growth.
Search News
Popular Tags
Industry Overview
The global commercial kitchen equipment market is projected to reach $112 billion by 2027. Driven by urbanization, the rise of e-commerce food delivery, and strict hygiene regulations.