FDA Final Rule: AI Diagnostic Devices Require Bias Assessment for US Market
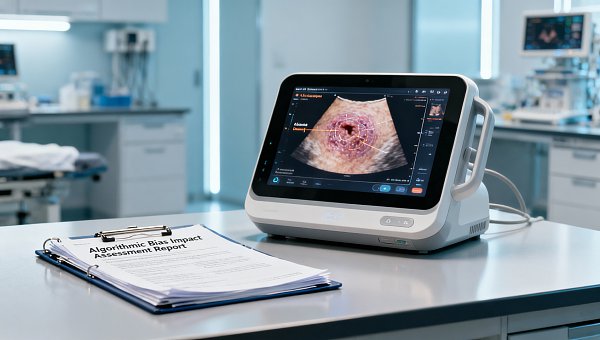
FDA’s April 25, 2026, final guidance on AI/ML-based SaMD introduces a mandatory algorithmic bias impact assessment for AI diagnostic devices entering the U.S. market — directly affecting manufacturers of portable ultrasound, dermatoscopes, and fundus analyzers, especially those exporting from China.
Event Overview
On April 25, 2026, the U.S. Food and Drug Administration (FDA) published the final version of its Artificial Intelligence and Machine Learning–Based Software as a Medical Device (AI/ML-Based SaMD) Enforcement Guidance. Under this guidance, all AI-powered diagnostic medical devices subject to 510(k) or De Novo premarket review — including portable ultrasound systems, dermatoscopes, and retinal imaging analyzers — must submit a third-party-verified ‘Algorithmic Bias Impact Assessment Report’ as part of their application. The report must include empirical testing results across race, sex, and age subgroups. The requirement takes effect immediately upon publication of the final guidance.
Industries Affected
Direct Exporters of AI-Enabled Medical Devices
Manufacturers based in China and other non-U.S. jurisdictions that supply AI diagnostic devices to the U.S. market are directly impacted. Because the new requirement applies at the premarket submission stage, these firms must now integrate bias testing into clinical validation protocols — adding measurable time and resource overhead before regulatory filing.
Contract Manufacturers & OEM Partners
Contract manufacturers producing AI-integrated hardware (e.g., embedded processors, imaging modules) for branded SaMD vendors face upstream demand shifts. Their quality documentation and design history files may now need to support bias-related data traceability — particularly where algorithm training data sourcing or model update mechanisms are involved.
Regulatory Consultancy & Third-Party Verification Providers
Organizations offering FDA submission support or conformity assessment services must now validate their capacity to conduct or oversee bias impact assessments per FDA-defined parameters. This includes methodological alignment with subgroup stratification, statistical power reporting, and transparency in dataset provenance — all subject to FDA scrutiny during review.
What Relevant Companies or Practitioners Should Focus On — And How to Respond
Monitor official FDA communications on implementation timelines and acceptable assessment methodologies
The final guidance does not specify standardized test protocols or thresholds for acceptable bias magnitude. Companies should track upcoming FDA webinars, draft Q&A documents, and updates to the Digital Health Center of Excellence resources — as these will clarify expectations for evidence sufficiency and verification rigor.
Prioritize bias assessment readiness for high-priority U.S.-bound product lines
Given the reported 3–5 week extension in submission preparation time, exporters should identify which devices are scheduled for 510(k) or De Novo submission in H2 2026 and beyond — then allocate internal or external resources to initiate bias testing early, especially for products with known demographic imbalances in training datasets.
Distinguish between policy signal and operational requirement
This is not a voluntary best practice but a binding condition for market access. Firms currently relying on legacy clinical validation packages — even if previously accepted by FDA — must treat bias assessment as a non-negotiable component of future submissions, not an optional add-on.
Update cross-functional coordination between R&D, clinical affairs, and regulatory teams
Because bias testing requires coordinated access to de-identified patient data, model versioning logs, and subgroup labeling frameworks, companies should formalize handoff procedures and documentation standards across departments — beginning now, ahead of next submission cycles.
Editorial Perspective / Industry Observation
From an industry perspective, this guidance signals a structural shift — not just a procedural update. It reflects FDA’s institutional move toward outcome-oriented oversight of AI performance across real-world population diversity, rather than solely technical validation under controlled conditions. Analysis来看, it is less about immediate enforcement penalties and more about establishing baseline accountability for health equity implications of AI diagnostics. Current more appropriate understanding is that this represents an enforceable entry gate, not a future aspiration. Continued attention is warranted because FDA has indicated plans to expand bias evaluation requirements to postmarket surveillance in subsequent iterations.
Conclusion
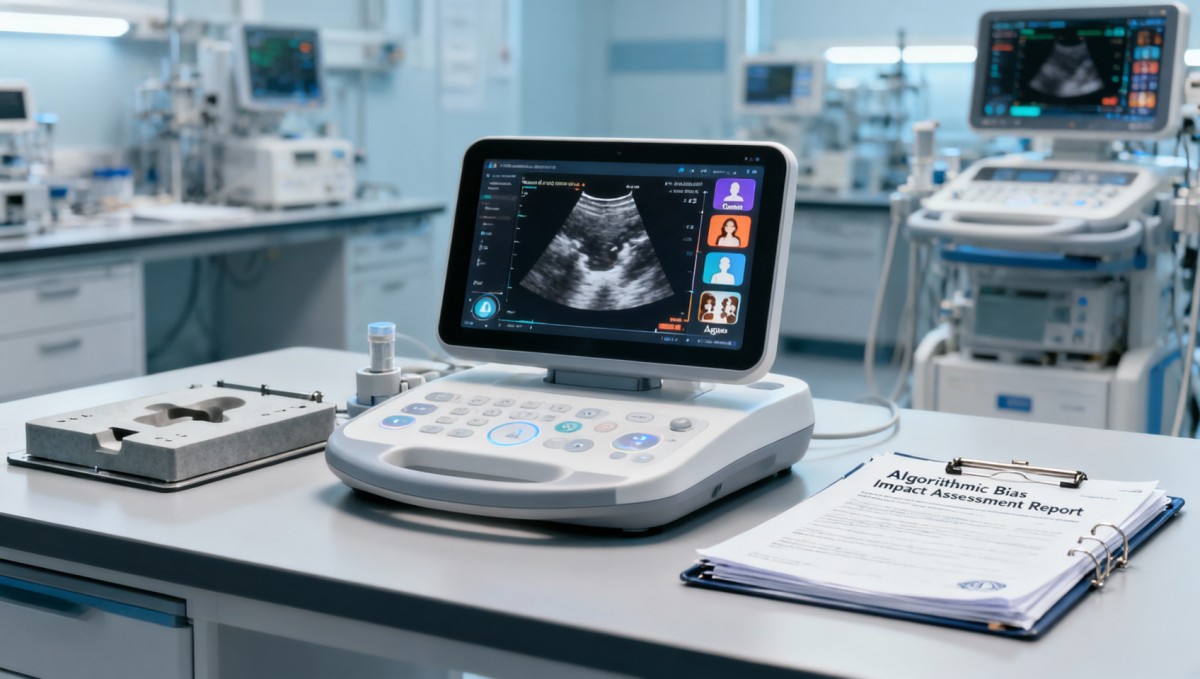
While narrowly scoped to premarket submissions for specific AI diagnostic device categories, this FDA action sets a precedent for algorithmic transparency and demographic accountability in regulated digital health. It is neither a temporary pilot nor a jurisdictionally isolated rule — but a foundational element of how AI-enabled medical devices will be evaluated in the U.S. going forward. For stakeholders, the current priority is not speculation about broader applicability, but precise alignment with the stated scope: race, sex, and age dimensions; third-party verification; and integration into existing 510(k)/De Novo workflows.
Information Sources
Main source: U.S. FDA, Artificial Intelligence and Machine Learning–Based Software as a Medical Device (AI/ML-Based SaMD) Enforcement Guidance, final version issued April 25, 2026.
Note: Ongoing developments — including FDA-issued interpretation documents, acceptance criteria for third-party verifiers, and potential extensions to Software-in-a-Device (SiD) configurations — remain under observation.
Recommended News
Popular Tags
Global Trade Insights & Industry
Our mission is to empower global exporters and importers with data-driven insights that foster strategic growth.
Search News
Popular Tags
Industry Overview
The global commercial kitchen equipment market is projected to reach $112 billion by 2027. Driven by urbanization, the rise of e-commerce food delivery, and strict hygiene regulations.